“It’s tough to make predictions, especially about the future.” These words, attributed to Yogi Berra, are a humorous way of saying that we can remember the past and live in the present—but what lies ahead exists in a fog of uncertainty.
In medicine, it’s important to manage expectations, since no treatments come with absolute guarantees. Until recently, medical professionals leaned on published statistics to help patients understand the chance of success as well as side effects. Data is good for calculating probability, but it would be better if there were a method to base prediction on a patient’s own anatomy.
Finally, there’s a way to do so, using multiparametric MRI (mpMRI) to help prostate cancer patients know what to expect if they have a prostatectomy. The patient wants to know if he will be incontinent (leaking urine) after surgery. Well, mpMRI can help manage expectations based on the patient’s own body. It all depends on a very small section of the urethra, or tube that carries urine from the bladder to the tip of the penis. Look at the illustration:
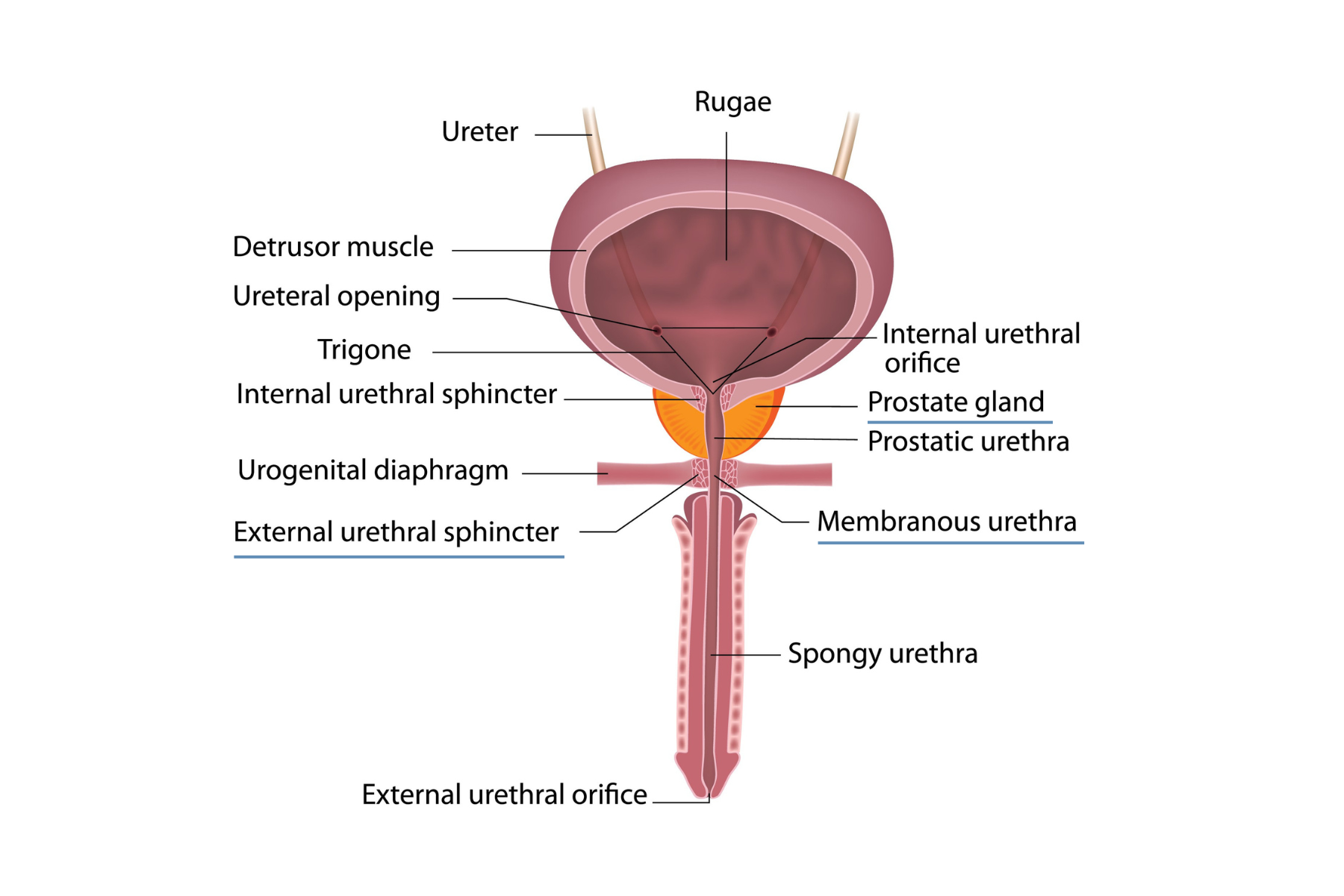
Locate the orange prostate gland. Above it is the large bladder (purple). You can see a thin purple tube from the bladder down through the middle of the prostate and continuing toward the tip of the penis. That is the urethra. When a surgeon performs a prostatectomy, the entire gland–including its part of the urethra—is removed. The surgeon must then pull the two ends of the urethra, one at the mouth of the bladder and the other at the top of the penis, together and stitch them to each other. In the diagram, notice the line pointing to the external urethra sphincter. This sphincter is a tiny muscle that controls urine flow. When the two separate ends of the urethra are stitched together, the surgeon makes every effort to avoid damaging that sphincter.
The reason to preserve the sphincter is because the shortest, narrowest part of the urethra runs through it. It’s a very small, narrow section called the membranous urethra. It’s shorter in some men than others. In the illustration, a line points to it where it’s surrounded by the external urethra sphincter. If the sphincter is damaged during surgery, so is the membranous urethra, which in turn can lead to post-surgical incontinence.
It turns out that the length of the membranous urethra has a bearing on the likelihood of incontinence. The shorter it is, the more likely it will be damaged during surgery and result in urine leakage. If a patient knows in advance that his membranous urethra is quite short, it might be enough for him and his doctor to consider an alternative to surgery rather than risk incontinence.
MRI reveals the length of the membranous urethra
Predicting incontinence is no longer a matter of statistical probability, thanks to a 2022 study published by Lamberg, et al. in the journal Radiology. The research team noted, “The ability to predict continence after [radical prostatectomy] could substantially aid physicians and patients when making treatment recommendations or decisions.” The study involved the cases of 586 PCa patients who had prostatectomy and who had urinary function records for 3, 6 and 12 months after surgery. All men had MRI-based measurements of their membranous urethra performed before surgery.
The authors found that longer preoperative membranous urethra length predicted better recovery of urinary control after surgery, while shorter length predicted incontinence (defined as use of adult diapers or more than one urinary pad per day). Thus, mpMRI can offer foreknowledge of a patient’s future, allowing him and his doctor to discuss not only how best to control his cancer, but also how to preserve his quality of life after treatment.
For more information on how mpMRI can help prostate cancer patients make treatment decisions, visit our website or contact the Sperling Prostate Center.
NOTE: This content is solely for purposes of information and does not substitute for diagnostic or medical advice. Talk to your doctor if you are experiencing pelvic pain, or have any other health concerns or questions of a personal medical nature.


