Transperineal Laser Ablation (TPLA) for Benign Prostatic Hyperplasia (BPH)
What is Transperineal Laser Ablation?
Transperineal Laser Ablation (TPLA) is a new FDA-cleared treatment to relieve the urinary symptoms of aging-related prostate enlargement called BPH.
TPLA uses laser-generated heat to ablate (destroy) targeted tissue. This causes strategic prostate areas to die, shrink, and eventually be absorbed by the body, reducing the size and volume of the prostate. As the prostate gland shrinks, the urethra naturally widens for normal urine flow.
Unlike other procedures that enter the prostatic urethra through the penis, TPLA inserts a slender laser fiber into the prostate through the perineum (skin below the scrotum). This is why it is called transperineal, meaning “through the perineum.” Local anesthetic is used to numb the perineum and the prostate.
TPLA is minimally invasive and avoids damage to key urinary and sexual structures. Treatment success is lasting, and side effects are rare. See published research at the end of this page.
How is the treatment done?
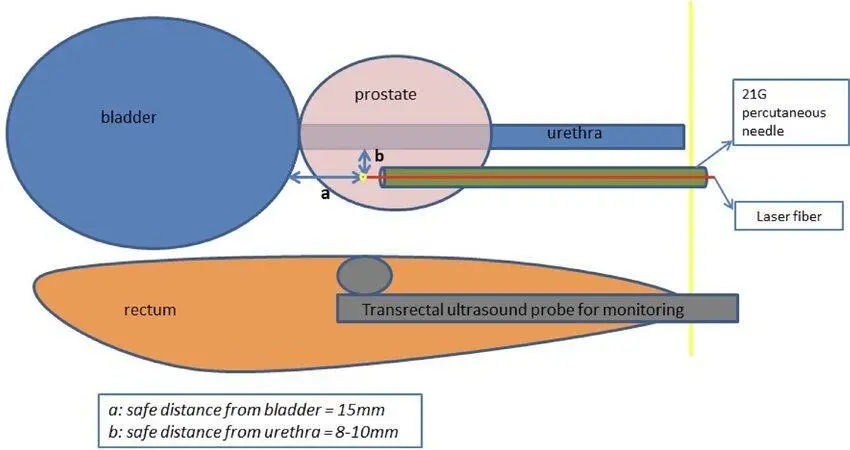
In order to plan treatment, mpMRI is used to identify the most strategic areas to ablate. Real-time transrectal ultrasound (TRUS) guides and confirms placement of the laser fiber. This combined imaging assures accurate planning, delivery, monitoring and confirmation of the treatment in real time.
This illustration[i] shows placement of the laser fiber (red line) and TRUS, which confirms safe distance from bladder and urethra to avoid damage to these structures.
To understand why TPLA is safe and effective with few-to-no side effects, let’s review BPH.
What is Benign Prostatic Hyperplasia (BPH)?
Benign Prostatic Hyperplasia (BPH), also called prostate enlargement, is a common noncancerous condition of the prostate gland that can occur as men age. In fact, roughly half of men between 50-60 years old have BPH, and it becomes more prevalent as men become older. It is estimated that 80% of men over age 70 have BPH.
Is BPH dangerous?
BPH is itself is not a dangerous condition. In fact, many men who have BPH may not know it because they don’t have bothersome symptoms. But the symptoms can pose health risks.
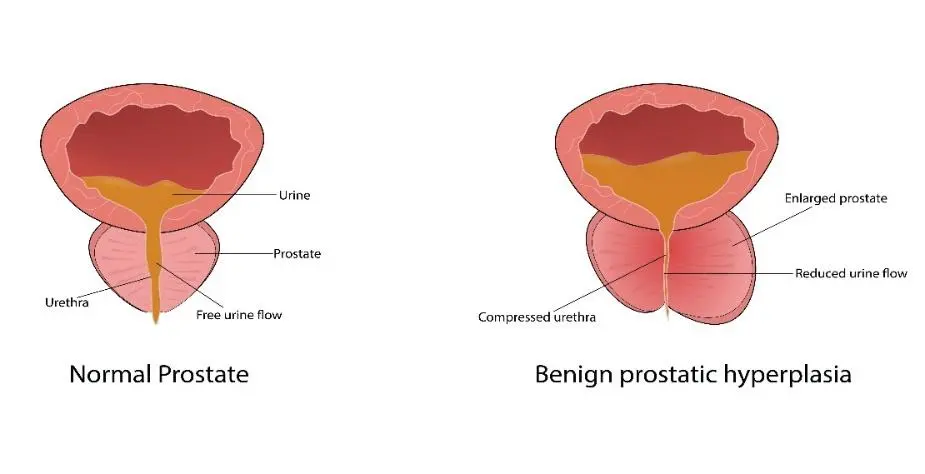
As gland grows bigger and bulkier, it compresses (squeezes) the passage that carries urine from the bladder through the prostate toward the penis. This passage is called the urethra. As pressure on the urethra increases, it can make urination difficult. See illustration.
The inability to fully empty the bladder is called retention. Retention poses a health risk. It increases the chances of urinary tract infections (UTIs). Bladder stones may develop. More seriously, urine can back up into the kidneys. If kidney damage occurs, there can be chronic infections or even kidney failure.
Are there early symptoms of BPH?
There are early symptoms, or warning signs, that BPH is occurring. These include
- Frequent urination or frequent sense of urgency
- Increased nighttime urination that disrupts sleep
- Difficulty starting to urinate
- Inability to completely empty the bladder
- UTI (urinary tract infection)
- Kidney infection
- Bladder stones
As with all medical conditions, the earlier BPH is diagnosed, the more treatable it is.
How is BPH treated?
There are several approaches to treating BPH. Treatment choice depends on how big the prostate is, how bad the symptoms are, and patient preference including side effect concerns.
- Medications –Some medications relax the prostate muscles and bladder neck to increase urine flow. Some act to block the hormone changes that lead to gland enlargement, so over time prostate size reduces. A combination of drugs may be used.
- Minimally invasive outpatient procedures – There are outpatient procedures to widen the urethra from the inside. One approach is to ablate (destroy) excess tissue that lines the urethra (urethral lining) using water vapor (steam). Another approach uses implants to hold prostate tissues away from the urethra.
- Surgical procedures – There are two standard surgical approaches to widen the urethra by “carving” a wider opening from the inside. Both are done by passing instruments through the tip of the penis into the urethra. One approach is a TURP (Transurethral Resection of the Prostate) which uses a special instrument to break up and remove excess tissue. The other approach uses a specific type of laser (usually either GreenLight or Holmium) that vaporizes tissues using very high heat.
How does Transperineal Laser Ablation (TPLA) differ from the above treatments?
Transperineal Laser Ablation is a new way to relieve the urinary symptoms of BPH. Unlike vaporization, uses a lower heat temperature that causes targeted tissue to die, shrink, and eventually be absorbed by the body. This process is called coagulation. It should not be confused with the GreenLight or Holmium laser types that use very high heat to vaporize tissue inside the urethra.
Procedures to widen the urethra from the inside are done by entering the gland through the penis. They literally either carve a larger passage, or create a wider opening using a permanent implant to pull tissue back.
However, TPLA is done through the perineum. It does not involve entering the urethra or damaging the urethral lining. Instead, coagulating strategically targeted areas gradually reduces the gland to a smaller volume. This takes pressure off the urethra. The passage naturally widens.
TPLA does not affect urinary or sexual function.
What are the benefits of Transperineal Laser Ablation for BPH?
Image-guided TPLA offers the following benefits:
- Outpatient procedure
- Local anesthesia with or without conscious sedation
- Entry through the perineum avoids damaging the urethral lining
- Temperature monitoring in real time
- MRI-confirmation of treatment zone and ablation effect
- Very rapid recovery time and return to normal activities
- No surgery or implants
Treatment effects:
- The urethra widens naturally as the volume of the prostate shrinks
- Very low risk of urinary side effects
- Very low risk of erectile dysfunction
- Success is durable
What does research show?
Studies provide a very favorable profile of Transperineal Prostate Ablation for BPH.
- ✓ “TPLA showed promising results in relieving obstructive symptoms, while preserving and even improving erectile and ejaculatory function, suggesting that it could be a valid option for young patients strongly interested in maintaining ejaculation.”[ii]
- ✓ “TPLA is an effective and minimally invasive treatment for LUTS/BPE [lower urinary tract symptoms/benign prostate enlargement], offering significant symptom relief, improved urinary flow, and preserved sexual function. Compared to TURP, TPLA provides advantages in ejaculatory function preservation, shorter operative time, and reduced hospital stay.”[iii]
- ✓ “TPLA for symptomatic BPH produced durable benefits across a range of clinical outcomes and was well tolerated in follow-up at median duration of 57 months.”[iv]
- ✓ “Transperineal Laser Ablation of the Prostate [TPLA] emerged as an ultra-minimally invasive ejaculation-sparing procedure, showing promising functional results, with a good safety profile.”[v]
- ✓ “TPLA is a safe and feasible treatment for men with LUTS due to BPO [benign prostatic obstruction]. TPLA can be performed in an outpatient setting under only local anaesthetics. Functional and quality of life outcomes improved significantly at 12 months, and erectile function remained stable.”[vi]
The Sperling Prostate Center now offers TPLA for the treatment of urinary symptoms due to benign prostatic hyperplasia (BPH). We are proud that our team of experts now includes Dr. Eric Walser, a recognized pioneer and published author on TPLA for BPH as well as prostate cancer.
NOTE: This content is solely for purposes of information and does not substitute for diagnostic or medical advice. Talk to your doctor if you are experiencing pelvic pain, or have any other health concerns or questions of a personal medical nature.
References
[i] Illustration from Tzelves, Lazaros & Nagasubramanian et al. (2023). Transperineal laser ablation as a new minimally invasive surgical therapy for benign prostatic hyperplasia: a systematic review of existing literature. Therapeutic Advances in Urology. 15. 10.1177/17562872231198634. Licensed through https://creativecommons.org/licenses/by-nc/4.0/
[ii] Alberti A, Lo Re M, Nicoletti R, Polverino P et al. Transperineal laser ablation in the management of benign prostatic hyperplasia: an updated systematic review and pooled analysis. Prostate Cancer Prostatic Dis. 2025 Mar 12.
[iii] Ibid.
[iv] Patelli G, Altieri VM, Ierardi AM, Carnevale A et al. Transperineal Laser Ablation of the Prostate for Symptomatic Benign Prostatic Hyperplasia: Long-Term Follow-Up in 40 Patients. J Vasc Interv Radiol. 2024 Aug;35(8):1187-1193.
[v] Alberti A, Lo Re M, Nicoletti R, Polverino P et al. Transperineal laser ablation in the management of benign prostatic hyperplasia: an updated systematic review and pooled analysis. Prostate Cancer Prostatic Dis. 2025 Mar 12.
[vi] Van Kollenburg R, Ibid.