Transperineal Laser Ablation (TPLA) for Prostate Cancer
What is Transperineal Laser Ablation (TPLA)?
Transperineal Laser Ablation is a new way to apply precision laser for the focal ablation (destruction) of localized prostate cancer tumors. It is a safe and effective minimally invasive approach. It is done as an outpatient procedure with local anesthesia.
Transperineal Laser Ablation has unique features that set it apart from other focal treatments.
What is unique about Transperineal Laser Ablation?
Two factors make Transperineal Laser Ablation unique. The first is the pathway used to direct precisely targeted laser to the tumor. Transperineal means “through the perineum”. The treatment is done by inserting a thin laser fiber through the perineum (outer skin below the scrotum) directly into the core of the tumor.
An advantage of this pathway is a significantly lower risk of infection. Also, local anesthesia numbs the perineum as well as the prostate nerves, assuring patient comfort in addition to safety.
The second factor is uniquely integrated image guidance. Like other focal ablation methods for prostate cancer, Transperineal Laser Ablation is image-guided. Our unique feature is the combined use of two imaging technologies, advanced multiparametric MRI (mpMRI) plus transrectal ultrasound (TRUS), for ultimate accuracy.
How is the treatment done?
mpMRI is used to identify the location and size of the tumor in order to guide the treatment plan, and confirm success. Real-time transrectal ultrasound (TRUS) guides and confirms placement of the laser fiber. This special combination assures precision planning, delivery, monitoring and confirmation of the treatment in real time.
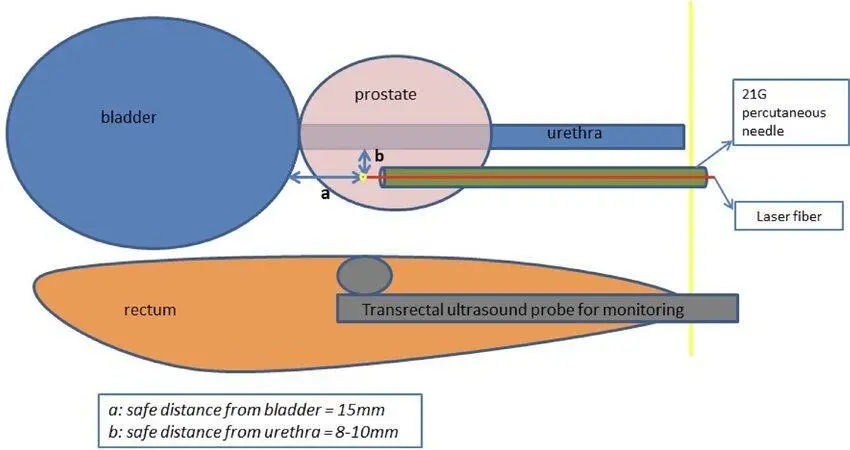
This illustration[i] shows placement of the laser fiber (red line). TRUS confirms safe distance from the bladder and urethra to avoid damage to these structures.
Benefits of Transperineal Laser Ablation
Transperineal Laser Ablation offers all the benefits of focal therapy for localized prostate cancer:
- Outpatient procedure
- Very low risk of urinary side effects
- Very low risk of erectile dysfunction
- Effective cancer control of the index lesion (primary tumor)
- MRI-confirmation of treatment zone and ablation effect
- Very rapid recovery time and return to normal activities
- No surgery or radiation
In addition, the transperineal pathway significantly reduces the risk of infection.
What does research show?
A featured poster abstract at the April 2025 annual meeting of the Society of Interventional Radiology is the most recent study.[ii] Dr. Eric Walser presented 1-year follow up data on 158 patients whose localized prostate cancer was focally treated using Transperineal Laser Ablation (TPLA). The data was pooled from three international clinics in the U.S. and Europe.
The authors concluded that TPLA is safe, durable and cost-effective for patients with organ-confined prostate cancer. With no significant treatment side effects, the data showed that Transperineal Laser Ablation does not impact quality of life.
One of the co-authors, Dr. Katelijne de Bie (Vrije Universiteit, Amsterdam) said in an interview, “Urinary symptoms and erectile function did not change after therapy, so it does implicate no significant effect on sexual or urinary function in our group. There were a small number who experienced retrograde ejaculation after the treatment, and some patients with transient urgency. But there are no patients with incontinence, so that is a huge difference compared to radical prostatectomy.”[iii]
Transperineal Laser Ablation at the Sperling Prostate Center
Thanks to the addition of Dr. Eric Walser to our team, the Sperling Prostate Center is proud to be a forerunner in offering Transperineal Laser Ablation. Dr. Walser also brings expertise in prostate imaging and MRI-guided focal treatments for localized prostate cancer. Going forward, this exciting new collaboration will focus on advancing prostate imaging and treatment and improving men’s health.
In addition, our Center also provides Focal Laser Ablation and Focal TULSA-PRO, Drs. Sperling and Walser work with each patient to qualify him for focal treatment, and to help him choose which method is the best fit for his disease and lifestyle.
Are you a candidate for TPLA?
References
[i] Illustration from Tzelves, Lazaros & Nagasubramanian et al. (2023). Transperineal laser ablation as a new minimally invasive surgical therapy for benign prostatic hyperplasia: a systematic review of existing literature. Therapeutic Advances in Urology. 15. 10.1177/17562872231198634. Licensed through https://creativecommons.org/licenses/by-nc/4.0/
[ii] Abstract No. 258 ? FEATURED ABSTRACT MRI-Directed Ultrasound-Guided Transperineal Focal Laser Ablation (TPLA) for Prostate Cancer: One-Year Follow-up of 158 Patients. Walser, E. et al. Journal of Vascular and Interventional Radiology, Volume 36, Issue 3, S119
[iii] “A new ablation technique for prostate cancer is seeing international success.” SIR Today, Mar. 30, 2025. https://irq.sirweb.org/sirtoday/abstract-258/
NOTE: This content is solely for purposes of information and does not substitute for diagnostic or medical advice. Talk to your doctor if you are experiencing pelvic pain, or have any other health concerns or questions of a personal medical nature.