Prostate Zone Anatomy, Prostate Cancer and Imaging
By: Dan Sperling, MD
The prostate gland is composed of different types of tissue, divided into zones:
- The peripheral zone (PZ) contains the majority of prostatic glandular tissue. The largest area of the peripheral zone is at the back of the gland, closest to the rectal wall. When a doctor performs a digital rectal exam (DRE) it is the back surface of the gland he is feeling. This is important because about 70-80% of prostate cancers originate in the peripheral zone.
- The central zone (CZ) is the area that surrounds the ejaculatory ducts. Only a very small percentage of prostate cancers begin here (less than 5%) and are thought to be more aggressive and more likely to invade the seminal vesicles.
- The transition zone (TZ) surrounds the urethra as it enters the prostate gland. It is small in young adults, but it grows throughout life, taking up a bigger percentage of the gland, and is responsible for benign prostatic hyperplasia (BPH, or normal gland enlargement that occurs with aging but can cause urinary problems). Roughly 20% of prostate cancers begin in this zone.
Prostate anatomy showing PZ, CZ and TZ:
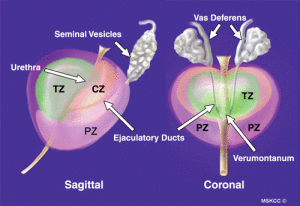
The Sagittal view is from the side, with the back of the PZ toward the rectal wall. The Coronal view is from the top, showing the left and right sides of the gland.
Image from Geneva Foundation for Medical Education and Research at http://www.gfmer.ch/selected_images_v2/detail_list.php?cat1=13&cat2=87&cat3=0&cat4=11&stype=n. Permission applied for.
Unlike ordinary ultrasound, multiparametric magnetic resonance imaging (mpMRI) is clearly able to depict the three zones of the gland, and to differentiate between healthy vs. diseased tissue. In addition, mpMRI can detect significant prostate cancer in any of the zones, and show any existing extracapsular extension (tumor at or beyond the edge of the prostate capsule).
There is a growing body of evidence that prostate cancers exhibit difference features depending on from which zone they originate. A 2014 study from Stanford University (California) examined biological differences between peripheral and transition zone prostate cancer[i]. The authors had access to records, including long-term clinical updates, on 1354 prostate cancer patients who underwent radical prostatectomy. Keep in mind that surgically removed glands are analyzed microscopically for biologic details on the prostate cancer they contain, so the zonal location was known as well as specific disease information). The research team discovered:
- Patients with TZ cancer had higher average pre-operative PSA values and larger total cancer volume (7.1 cc vs. 3.8 cc in PZ cancers).
- Patients with TZ cancer had decreased odds of seminal vesicle invasion and extracapsular extension.
- Patients with TZ cancer had reduced risk of cancer recurrence.
Therefore, they concluded that even though TZ tumors appear to be larger and lead to higher PSA test results, they were associated with favorable features when analyzed after surgery, and had better rates of recurrence-free survival.
A study from the same institution 14 years earlier examined specific differences between TZ and PZ tumors. [ii] Out of 148 consecutive cases of TZ cancer treated by radical prostatectomy (RP), 79 were matched by total cancer volume to 79 cases of strictly peripheral zone cancer for comparison purposes. Postoperatively, biochemical disease failure was assessed by an ultrasensitive PSA of 0.07 ng/ml and increasing.
Of the 148 cases of TZ cancer, the following characteristics were reported:
- 80% organ confined disease
- 70% stage T1c impalpable disease (not detected on DRE)
- 63% positive initial biopsy
- 62% unilateral cancer in the TZ
- 52% a secondary tumor only in the PZ
- 61% preoperative PSA 10 ng/ml or greater
- 36% cancer volume greater than 6cc
- 24% at least 50% Gleason grade 4/5 cancer
The authors found that 15% of patients had capsular penetration upon surgery, 29% had anterior positive surgical margins, 2.7% seminal vesicle invasion and 3.4% spread to lymph nodes. When 79 TZ tumors were matched by volume with 79 PZ tumors, there were no differences in percent Gleason grade 4/5, serum PSA or prostate weight. However, differences in clinical stage T1c to T2c and organ confined cancer were highly significant. At five years follow up, there was a large difference between groups with regard to undetectable PSA; patients with TZ tumors had a 71.5% rate of undetectable PSA, but those with PZ tumors had just under half (49.2%) with undetectable PSA. The authors concluded that the source of the differences between the two cancers “must be sought at the molecular level unless anatomical location alone explains the differences in progression.” They recommend that when RP specimens are sent to the lab for evaluation, pathologists should differentiate location (TZ or PZ) in their reports.
A very early study (1988) sheds light on the different cellular structure of TZ prostate cancer based on laboratory examination of 88 surgically removed glands where the zone of origin could be identified.[iii] The study reports that 68% arose in the PZ, 24% in the TZ and 8% in the CZ. Of the TZ cancers (21 cases), two-thirds “showed a distinctive histologic appearance; they were made up of columnar clear cells lining glands of widely variable size and contour. The transition zone boundary appeared to act as a barrier to the spread of non-transition zone carcinomas.” This led the authors to conclude that prostate cancer may arise in the region of the prostate that is susceptible to benign prostatic hyperplasia. Perhaps this accounts, in part, for why transition zone tumors seem to correlate with lower aggression compared to PZ cancers.
As multiparametric is able to identify in which zone prostate cancer occurs, the data from studies that characterize the differences, including aggression level, of zonal cancers, knowing the location based on imaging may suggest that certain genomic tests be applied to biopsy samples to further assess the risk level of a PZ cancer, for example, which appears to have a higher rate of biochemical failure than a TZ tumor of the same volume. Research data points to the fact that all zonal cancers are not alike, and may require treatment to match the disease.
[i] Lee JJ, Thomas IC, Nolley R, Ferrari M et al. Biologic differences between peripheral and transition zone prostate cancer . Prostate. 2014 Oct 18. Epub ahead of print. doi: 10.1002/pros.22903 PMID: 25327466
[ii] Noguchi M, Stamey TA, Neal J, Yemoto C. An analysis of 148 consecutive transition zone cancers: clinical and histological characteristics. J Urol. 2000 Jun;163(6):1751-5.
[iii] McNeal J, Redwine E, Freiha F, Stamey T. Zonal distribution of prostatic adenocarcinoma: correlation with histologic pattern and direction of spread. Am J Surg Pathol. 1988 Dec;12(12):897-906.

