MRI/TRUS Fusion Biopsies
The Sperling Prostate Center offers a targeted MRI-Guided biopsy of suspected prostate tumors using two types of procedures:
- MRI-Guided Biopsy – Using advanced MRI images of a suspected tumor/tissue, Dr. Sperling performs a targeted prostate biopsy inside the MRI gantry.
- MRI/TRUS Fusion Biopsy – First an advanced MRI prostate image is obtained, annotated and recorded by the Sperling Prostate Center. Next, using special fusion technology, the recorded MRI image is fused with a live transrectal ultrasound by the Urologist who performs a MRI/TRUS fusion biopsy.
Why MRI/TRUS Prostate Biopsy
A critical component in accurate prostate tumor diagnosis and appropriate treatment is the ability to efficiently biopsy specific areas of the prostate. It’s estimated that over 1.5 million prostate biopsies are performed on men each year. As many as 1 million of them may be unnecessary1. Until now, conventional biopsies have been the standard of care when prostate cancer is suspected.
The issue is that a conventional biopsy can miss 30-40% percent of cancers2. Likewise, a conventional prostate biopsy may detect tumors that are not clinically relevant and could be just watched or at least treated less radically.
The problem is that conventional prostate biopsy technology has not changed much over the last 20 years. The procedure is performed using a handheld Ultrasound probe that provides only a small and often cloudy view of the prostate. In some ways a conventional prostate biopsy, though systematic on both sides of the gland, is a “blind” procedure that relies on probability (or sometimes even guesswork) as to the locations of the biopsy sampling.
Now thanks to Artemis, new technology from Eigen, physicians can fuse MRI and TRUS images to confidently sample precise areas of the prostate and to record biopsy locations for future reference in their diagnosis and management. While several other imaging modalities have been tested, most are cumbersome, expensive, and in some cases expose the patient to additional radiation or an inordinate number of biopsy samples.
The Artemis-MRI/TRUS Fusion function can help provide physicians and patients with more information about the exact location and extent of the disease. The result can lead to a more accurate diagnosis along with better information to help make a smarter, more individualized choice about prostate cancer management and follow up.
Today’s next generation, advanced MRI technology is combined with the proprietary protocol of the Sperling Prostate Center to produce high-resolution 3D images that can distinguish between normal and diseased tissue to help precisely pinpoint potential cancerous cells within the prostate. The result is better ability to identify and characterize prostate cancer, especially important in today’s changing landscape of smaller, lower risk tumors.
By fusing the MRI and live ultrasound images, a urologist can more effectively perform a targeted prostate biopsy of select tissue revealed by MRI imaging3. That means physicians and patients have the confidence that the tissue samples come from locations identified as highly suspicious. The result is a true TRUS targeted approach vs. the “blind” approach of a standard TRUS biopsy.
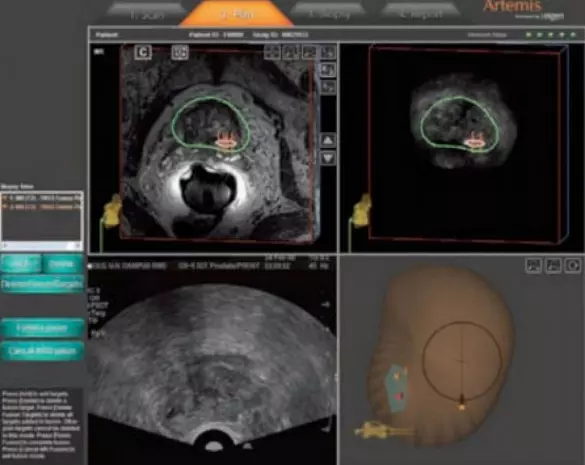
*IMPORTANT: The Artemis device is an FDA Cleared device for prostate imaging. However, the MRI Fusion Function is still pending FDA clearance.
MRI/TRUS Fusion Biopsy Overview
- The Most Sophisticated Prostate Biopsy: An Artemis-MRI/TRUS Fusion Biopsy ensures that your prostate examination and biopsy is performed utilizing the world’s most sophisticated TRUS based biopsy , including 3D visualization, navigational functionality, needle tracking and recording for future reference. This breakthrough technology provides patients and their doctor detailed, personalized information – creating an advanced prostate diagnostic procedure.
- Advanced Diagnostic Information: An Artemis-MRI/TRUS Fusion Biopsy allows physicians to examine, plan and record the biopsy – all through the power of 3D visualization. This detailed information helps the physician to target precise locations where suspicious tissue and/or prostate cancer tumors are suspected, thus providing advanced clinical information for diagnosis and, if necessary, treatment and follow-up.
- Information For A Better Treatment Decision: An Artemis-MRI/TRUS Fusion Biopsy provides clear, reliable information that can help patients and physicians make a better, more informed (and more individualized) decision about the course of care, whether it be watchful waiting, hormone therapy, targeted thermal ablation, nerve sparing robotic surgery, or radiation therapy.
- Long-Term Personalized Management: With an Artemis-MRI/TRUS Fusion Biopsy the actual location of your biopsy can be recorded and stored. The result is a baseline of prostate biopsy information that allows for future reference, confirmation and follow-up. In turn, this means better and more personalized longterm patient management.
- 3D Reporting: Artemis-MRI/TRUS Fusion using the Artemis technology provides easy to understand high definition 3D graphic reports that clearly identify the location of each biopsy sample. The result is more information to patients and physicians make the best, most informed, treatment decision possible.
MRI/TRUS Fusion Biopsy vs. Standard TRUS Biopsy
- Visualization: Artemis 3D visibility provides better imaging than standard 2D views.
- Planning: The Artemis planning module helps physicians to distribute the biopsy samples evenly based on the prostate sizes and shape.
- Navigation: The Artemis tracking arm facilitates precise needle tracking, helping to ensure your physician samples the exact target locations.
- Reporting: The Artemis software allows for the exact recording of the actual sample, making the known location and repeat biopsy easier and more accurate.
MRI/TRUS Fusion Biopsy Advantages
-
Precise prostate Imaging & Navigation: An Artemis-MRI/TRUS Fusion Biopsy offers the only true smart prostate biopsy procedure—providing your physician with 3D prostate visualization, precise needle tracking and biopsy location recording for future reference.
- Advanced Diagnostic Data: An Artemis-MRI/TRUS Fusion Biopsy allows physicians to examine, map, plan and record your biopsy. The detailed 3D provides precise location of suspicious tissue and/or cancer lesions. This results in advanced clinical information to aid in diagnosis, treatment and continuing care.
- Better Treatment Information: The Artemis-MRI/TRUS Fusion Biopsy provides clear, reliable information that can assist patients and physicians in making a more informed, individualized decision about the most appropriate course of care.
- 3D Patient Reporting: At the conclusion of the Artemis-MRI/TRUS Fusion Biopsy, Artemis yields an easy-to-understand, high-definition color report you can take home. It clearly identifies each biopsy sample location, along with more valuable information to help patients and physicians make the best, most informed treatment decision possible.
- Accurate Repeat Biopsy: With its unique biopsy location recording capability, your physician has the ability to re-biopsy the same locations in the gland or to sample other areas around any specific location. This helps ensure that any subsequent biopsies are more accurately sampled than ever before.
- Long-term Personalized Management: Since Artemis-MRI/Fusion Biopsy records the location of each biopsy sample, your physician is able to construct a personal baseline of data that greatly enhances future reference, confirmation and followup. The bottom line is better information for better long-term health care management.
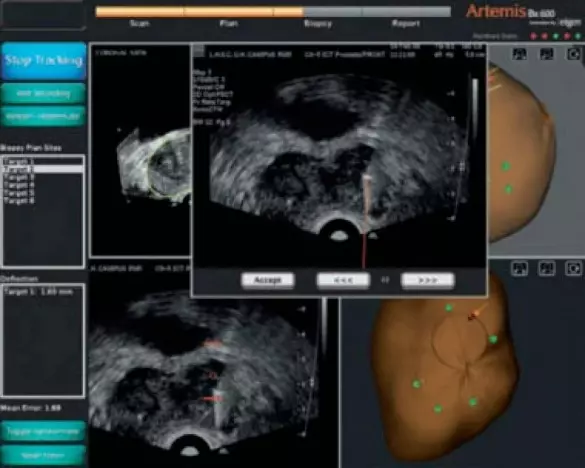
Artemis – Smart Prostate Biopsy Steps
- Prostate Scanning – 3D Image
- Biopsy Planning
- Navigation and Recording
- Biopsy Reporting
Prostate Scanning
The first step is for your doctor to take a 360° scan of your prostate using a standard 2D ultrasound system connected to Artemis. Next, Artemis automatically converts the standard 2D ultrasound image into an enhanced 3D prostate image. Your physician can easily adjust the prostate boundary and contour to customize the image even further.
The result is a clear 3D prostate rendering that provides full 3D rotational functionality along with real-time views of the prostate in multiple planes – coronal (top), sagittal (side) and transverse (front). The visualization experience is amazing, allowing your doctors to see the entire prostate as one clear complete image. The power of 3D helps to increase your physician’s ability to examine the prostate for abnormalities or suspicious areas that might otherwise not be detected. By seeing the gland in 3D it’s easier for your doctor to be sure the entire prostate is examined correctly. Likewise, it’s easy to find any areas of potential concern.
Artemis and MRI (An Optional Scanning Module)
The Magnetic resonance imaging (MRI) Fusion Module* allows physicians to integrate three images (MRI, 3D-Artemis rendering, and real-time ultrasound images) into one single visual.
MRI is a test that uses a magnetic field and pulses of radio wave energy to make pictures of organs and structures inside the body. In many cases MRI gives different information about structures in the body than can be seen with an ultrasound. MRI also may show problems that cannot be seen with other imaging methods.
The fusion function gives physicians the most sophisticated imagery and navigational ability available. It provides high resolution along with exact structural dimensional functionality. The result is a significantly enhanced prostate examination and biopsy sampling. Your physician now can have the confidence of precise needle placement in areas identified by the radiologist during the MRI scan.
The MRI fusion feature allows physicians to scale an exam and/or biopsy – from the simplest to the most advanced procedure – to meet patient needs. MRI fusion is typically useful in patients who require repeat biopsies or for patients with a negative biopsy and continued PSA escalation. MRI fusion is also helpful in patients with specific areas (or lesions) of concern of for patients with very low-risk or very high-risk disease. The optional fusion functionality allows your physician the ability to customize each procedure as needed. And it helps to simplify a busy practice by having one system that can handle every type of prostate exam and biopsy.
Planning
Step two is planning. Under the planning module Artemis automatically generates a standard 6 or 12 core biopsy template that systemically conforms to your prostate size and shape, creating a customized patient plan. Physicians can easily make adjustments to customize the standard plan or can create an “individualized biopsy plan”. If desired, physicians can simply turn the template feature off and follow their own biopsy plan. No matter what plan is followed the Artemis tracking function will simply record wherever the biopsy sample is taken, giving your doctor maximum flexibility and control at all times. Artemis also gives your physician the option to easily and precisely add additional biopsy samples in specific locations. This is helpful in hard to see and hard to reach areas of the prostate like the apex or anterior sections. Naturally, Artemis gives physicians the ability to target biopsy in areas of abnormalities and/or suspicious sites (both with or without the MRI fusion*). Finally the planning feature allows your physician the capability to perform a true prostate biopsy mapping by using 3D visualization to plan the needle placement and track actual samples sites.
Navigation and Recording
Step three is navigation and recording. Artemis allows physicians to achieve exact needle placement by using the system’s real-time dynamic needle track navigation capabilities. This unique software tracks the needle as the physician glides the ultrasound probe along each biopsy template. The software lets physicians precisely navigate where they want to take the sample by using Artemis’s XYZ navigation guidance process (much like a video game or GPS). Once the doctor aligns the ultrasound probe with the 3D template image, the probe can be temporarily locked in place and a biopsy sample is taken. Artemis then precisely records the location of the biopsy sample site for reporting. This unique software–hardware interface makes Artemis easy to learn and simple to use. Best of all, the tracking function give doctors the ability to revisit any and all previous biopsy sample sites. The process helps to eliminate blind-biopsies and guessing where the needle is.
If a patient has had a previous biopsy with Artemis, his physician can access the biopsy recording for repeat biopsy planning, including overlaying a previous prostate volume and actual biopsy site locations. This gives your doctor the ability to re-sample the same biopsy sites, sample different sites, or saturate a particular area. Most importantly, the tracking function can be used to conduct precise serial biopsy sampling for “Active Surveillance” patients. This important function can also help physicians manage patients who had a previous biopsy and patients who have already been treated for prostate cancer. Essentially, Artemis helps to create a long-term patient relationship by providing a sophisticated biopsy management platform that helps ensure that patients who return to the same clinic have their history of accurate biopsies locations recorded.
Biopsy Reporting
The Artemis reporting package provides exquisite visualization of the actual locations where the biopsies were taken. This information allows physicians and patients to clearly see where biopsy samples originated from and where additional sample site opportunities may exist. The report gives the physician high quality information for rebiopsy, targeted treatment and disease conformation or management. Likewise, the Artemis’ 3D pathology model is excellent for treatment planning especially in cases where a targeted ablation or nerve sparing procedure is being considered. Lastly, the 3D rendering is an excellent way for your doctor to communicate with you. Because of the high-end graphics, rich color and easy to understand advanced imagery the Artemis reports are both exciting and informative for you, the patient. The result is more information for you and a higher quality discussion about treatment options andactions. The report also sets a foundation for long-term relational management between you and your doctor regardless of diagnosis and/or treatment choice.
Who Should Consider a Prostate MRI
- Patients with a rising PSA level yet negative biopsy (Anastasiadis 2006; Lichy 2006). The detailed information provided by MRI can lead the doctor to the area most suspicious for disease, thereby increasing the chance of obtaining a comprehensive biopsy.
- Patients who have experienced a biopsy one or more times and want to improve the sensitivity of diagnosis for cancer, if present
- Patients looking to identify the precise size, location and extent of prostate cancer
- Patients looking to help confirm the stage and grade of their prostate cancer
- Patients looking to determine if their cancer is confined to the prostate, or if it has spread outside the walls of the prostate gland
- Patients who choose to monitor a low level of prostate cancer in order to hold off on treatment
- A patient’s radiation treatment therapy can be planned, as it is important that the radiation be concentrated on the affected area (Mizowaki 2002). An MRI can provide a clear picture in helping the oncologist guide the therapy that is most appropriate for a particular patient.
- Patients who are considering a radical prostatectomy, including a robotic procedure. An MRI can provide a clear picture in helping the urologists to guide the surgery to be effective while reducing morbidity (Hricak 2004; McClure 2010).
- Patient considering an ablation, including Laser, Cryoablation or HIFU (Morgan 2007)
- Patients considering a focal or targeted ablation treatment (Morgan 2007; Shukla 2007)
- Patients who have a local recurrence, indicated by a high PSA level, following a radical prostatectomy, radiation, Cryoablation, HIFU or Laser Ablation. MRI can evaluate the entire area for abnormal tissue.
MRI Guided Prostate Biopsy Risks
Biopsy Risks
A prostate biopsy has a slight risk of causing problems such as:
- Infection. This is more common in men who have undiagnosed prostatitis. Usually, taking antibiotic medication before the biopsy prevents an infection from developing.
- Bleeding into the urethra or bladder. This can cause a blood blister (hematoma), an inability to urinate, or a need to urinate often.
- Bleeding from the rectum. If you have a transrectal biopsy, you may experience a small amount of bleeding from your rectum for 2 to 3 days after the biopsy.
- An allergic reaction to the anesthetic medications used during the biopsy.
Note: A prostate gland biopsy does not typically cause any long term problems with erections and will not make a man infertile.
MRI Risks
- The MRI examination poses almost no risk to the average patient when appropriate safety guidelines are followed.
- Although the strong magnetic field is not harmful in itself, implanted medical devices that contain metal may malfunction or cause problems during an MRI exam.
- There is a very slight risk of an allergic reaction if contrast material is injected. Such reactions usually are mild and easily controlled by medication. If you experience allergic symptoms, a radiologist or other physician will be available for immediate assistance.
- Nephrogenic systemic fibrosis is currently a recognized, but rare, complication of MRI believed to be caused by the injection of high doses of gadolinium contrast material in patients with very poor kidney function.
* IMPORTANT: The Artemis device is an FDA Cleared device for prostate imaging. However, the MRI Fusion Function is still pending FDA clearance.
- AdMeTech Foundation. Prostate cancer crisis: key statistics. http://www.admetech.org/PCC/index.php . (2008).
- Ahmed HU, Kirkham A et al. Is it time to consider a role for MRI before prostate biopsy?. Nat Rev Clin Onc . 6. 197-206. (2009).

